Image
Best Practice magazine
A journal of dentistry, business and policy that shines a spotlight on Delta Dental network dentists.
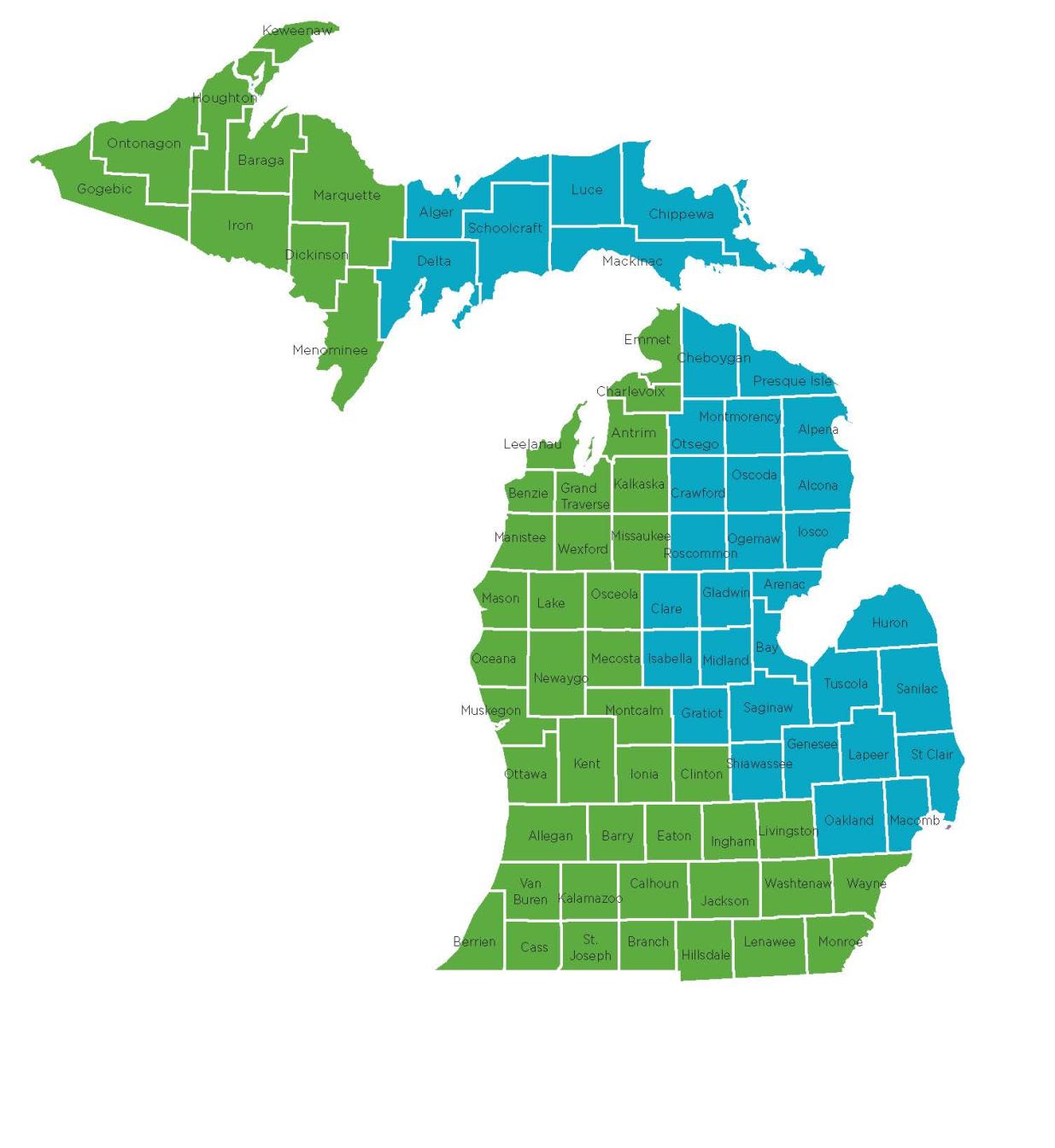
Do you know your provider representative?
Find your county and reach out today!
Image

Image

Counties by representative
Upper Peninsula
- Baraga
- Dickinson
- Gogebic
- Houghton
- Iron
- Keweenaw
- Marquette
- Menominee
- Ontonagon
Lower Peninsula
- Allegan
- Antrim
- Barry
- Benzie
- Berrien
- Branch
- Calhoun
- Cass
- Charlevoix
- Clinton
- Eaton
- Emmet
- Leelanau
- Grand Traverse
- Hillsdale
- Ingham
- Ionia
- Jackson
- Kalamazoo
- Kalkaska
- Kent
- Lake
- Lenawee
- Livingston
- Manistee
- Mason
- Mecosta
- Missaukee
- Monroe
- Montcalm
- Muskegon
- Newaygo
- Oceana
- Osceola
- Ottawa
- St. Joseph
- Van Buren
- Washtenaw
- Wayne
Wexford
Upper Peninsula
- Alger
- Chippewa
- Delta
- Luce
- Mackinac
- Schoolcraft
Lower Peninsula
- Alcona
- Alpena
- Arenac
- Bay
- Cheboygan
- Clare
- Crawford
- Genesee
- Gladwin
- Gratiot
- Huron
- Iosco
- Isabella
- Lapeer
- Macomb
- Midland
- Montmorency
- Oakland
- Ogemaw
- Oscoda
- Otsego
- Presque Isle
- Roscommon
- Saginaw
- Sanilac
- Shiawasee
- Tuscola